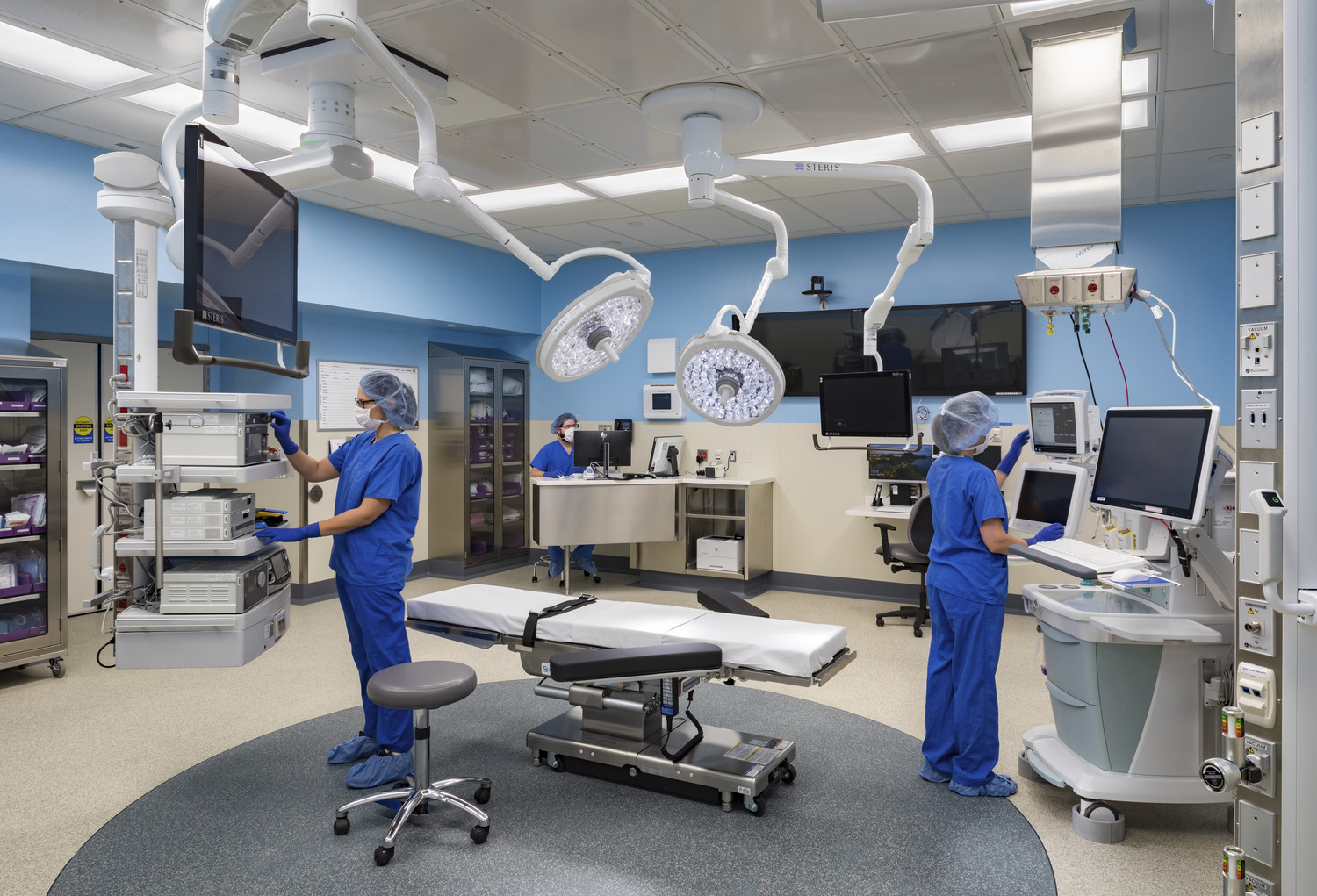
Acuity Adaptability: Larger rooms, staff culture shift among challenges

Fourth in a series of excerpts from the free executive guide, “Acuity Adaptability: Innovative Planning and Design for Responsive Healthcare Delivery.”
By Mike Zorich and Corey Gaarde
Acuity adaptable healthcare design – keeping a patient in the same room from admission to discharge – has many benefits, but it is not a perfect solution, nor is it a universal cure-all. Hospitals often face challenges in implementing acuity-adaptable design concepts. Some facilities or specialties are better able to absorb these drawbacks or overcome these challenges than others.
The problems may become more pronounced in larger facilities, where the introduction of acuity-adaptable design may reduce the number of beds and increase the time doctors and nurses spend walking from one wing of the acuity-adaptable unit to another. In addition:
- A fully acuity-adaptable room may need to be up to twice the size of a standard room, resulting in higher renovation costs and potentially fewer total rooms.
- Since all care must come to the patient, every piece of diagnostic and telemetry-monitoring equipment must be portable. This could entail additional significant cost.
- Acuity adaptability adds a level of complexity to the billing process and may require new charge codes or assessment of the level of care each day.
- Nurses and care providers must be able to offer any level of care a patient might require. Staff culture may present a major challenge if facility staff have trouble adapting.
These and other challenges and drawbacks must be weighed against the benefits for each facility considering an acuity adaptable model.
In the next blog, we will explore different specialties and settings that are more apt to benefit from acuity adaptability.
Previous: Acuity Adaptability: Benefits to patients, caregivers, and healthcare facilities
Next: Acuity Adaptability: Settings that benefit
For an unabridged version of this content, download the executive guide, “Acuity Adaptability: Innovative Planning and Design for Responsive Healthcare Delivery.” A recorded webinar on the topic is also available.