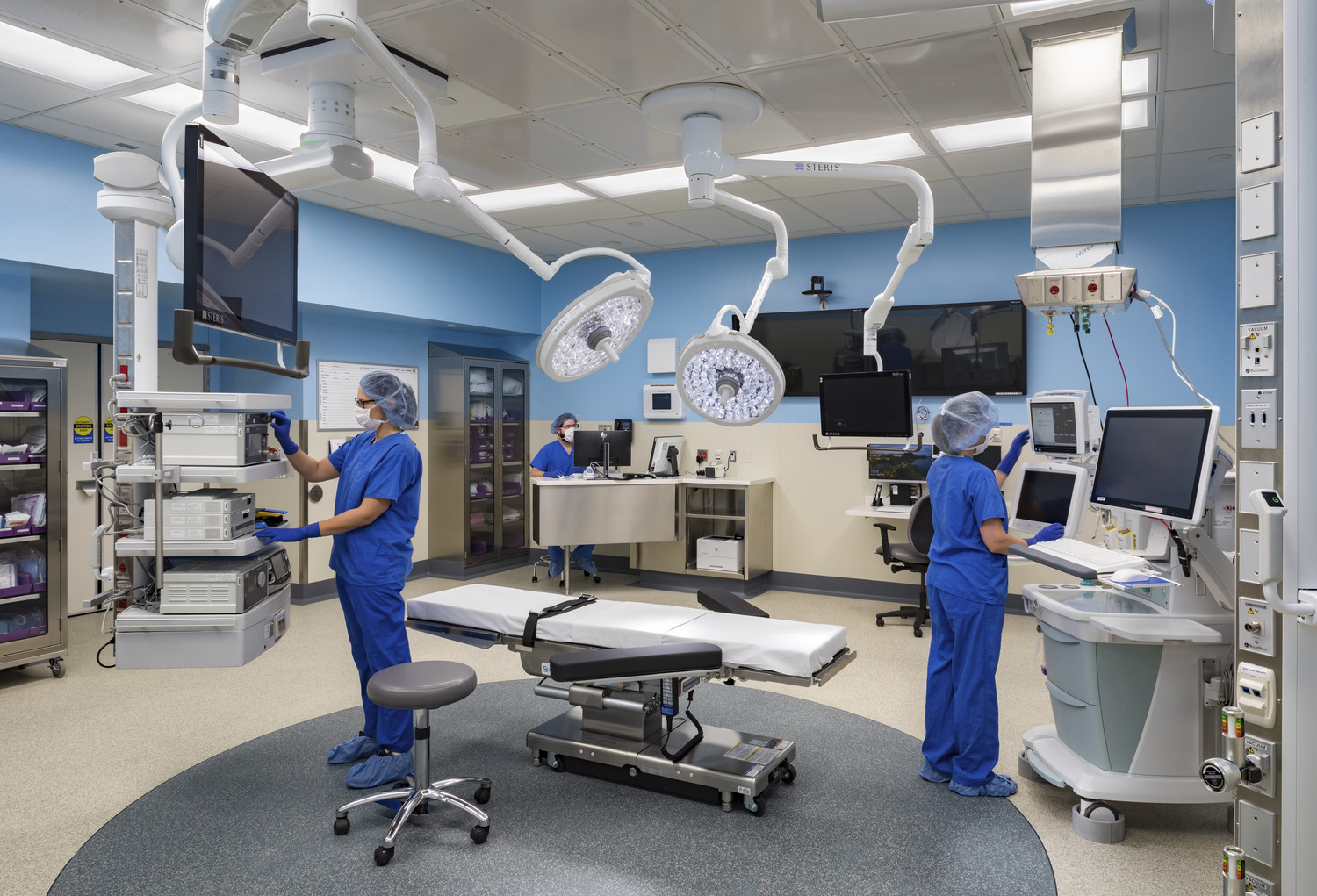
Resilience in Healthcare: 5 critical areas for reducing risk during a disaster

First in a series of excerpts from the IMEG executive guide, “The Importance of Healthcare Resiliency: Preparing Your Hospital for a Crisis.”
By Eric Vandenbroucke
Resilience in healthcare can only be served if your hospital is prepared to face the worst. By taking proactive steps and making concrete plans to further the disaster preparedness of your healthcare facility or system, you’ll be better equipped to answer the call of your community during dire situations.
In addition to being resilient to ever-more-frequent natural disasters, hospitals also must be prepared for other disruptions such as power outages, infrastructure failures, mass casualty events, infectious outbreaks, and cyber attacks – all of which impair their ability to provide lifesaving care to their vulnerable patient population. Without a clear plan and definitive course of action in place ahead of time, your hospital could be left scrambling to recover, putting patients and staff at risk and leaving your facility liable.
With such a broad range of threats that can occur, how can you ensure your hospital is adequately prepared? Further, assuming the requirements for healthcare resiliency will continue to evolve, how can you ensure your hospital stays adequately prepared?
Answering these questions first requires an understanding of four commonly accepted characteristics of infrastructure resiliency, as defined in 2009 by the National Infrastructure Advisory Council:
- Robustness: the ability to maintain critical operations and functions in the face of crisis. This includes the building itself, the design of the infrastructure (office buildings, power generation, distribution structures, bridges, dams, levees), or in system redundancy and substitution (transportation, power grid, communications networks).
- Resourcefulness: the ability to skillfully prepare for, respond to, and manage a crisis or disruption as it unfolds. This includes identifying courses of action and business continuity planning, training, supply chain management, prioritizing actions to control and mitigate damage, and effectively communicating decisions.
- Rapid recovery: the ability to return to or reconstitute normal operations as quickly and efficiently as possible after a disruption. Components of rapid recovery include carefully drafted contingency plans, competent emergency operations, and the means to get the right people and resources to the right place.
- Redundancy: having back-up resources to support the originals in case of failure.
Using these traits as a benchmark, you can begin to take an informed look at the main resiliency issues facing your healthcare facility:
- Structural integrity
- MEP infrastructure
- Physical security
- Mass casualty events and infectious outbreaks
- Cyber security
This is the first in a series of blog posts based on IMEG’s updated executive guide, “The Importance of Healthcare Resiliency: Preparing Your Hospital for a Crisis.” Other posts in the series, listed below, provide a brief look at the key areas noted above, which represent many of the most often overlooked and misunderstood aspects of hospital risk management.
- 3 questions to help define the structural integrity of your hospital
- 4 key areas of MEP resilience reduce healthcare facility risk during a natural disaster
- Enhance hospital security through CPTED principles
- Prepare for mass casualty events and infectious outbreaks
- Improve healthcare cyber security with holistic approach to technology design
- Bonus: 10 key areas for hospital disaster preparedness